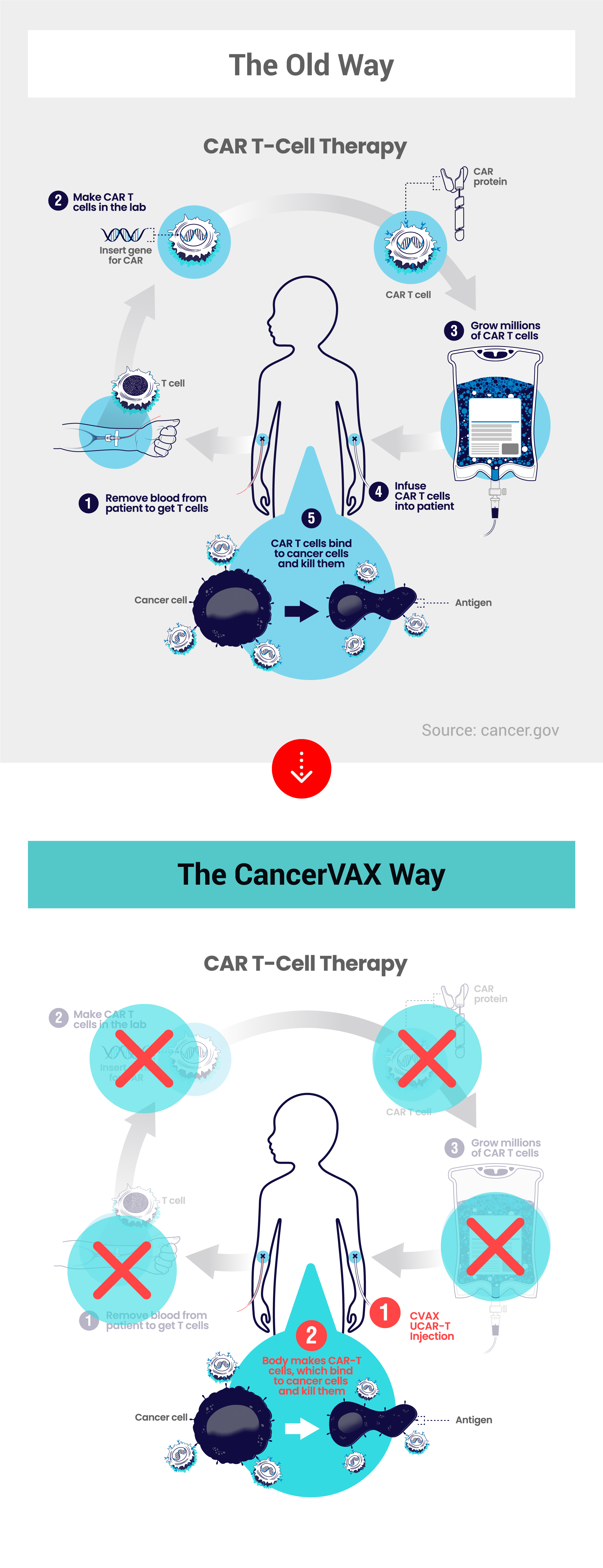
By leveraging cutting-edge bioengineering and molecular technologies, we are on a quest to develop innovative precision cancer immunotherapies. Inspired by the way COVID-19 vaccines train the body to recognize and destroy the coronavirus, we are developing cancer vaccines, also known as cancer immunotherapies, that uses the body’s immune system to fight cancer.